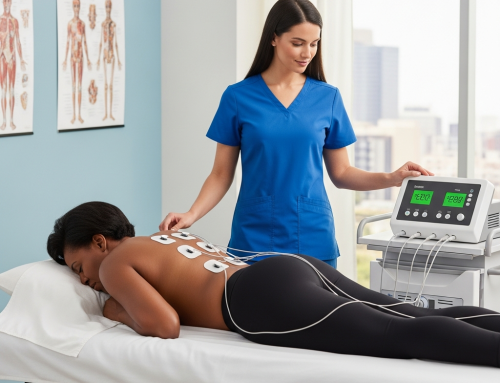
Whitehouse Car Wreck Doctor: When to Seek Treatment
You’re driving home from work on Route 31, maybe thinking about what’s for dinner or whether you remembered to pay the electric bill, when *bam* – some guy texting behind the wheel slams into your rear bumper. Your heart’s pounding, your neck feels… weird, and suddenly you’re standing on the side of the road wondering what the hell just happened.
Here’s the thing everyone tells you: “Oh, you look fine! The car barely has a dent.” Your neighbor, your coworker, maybe even the responding officer – they all seem to think that if you can walk away from an accident, you’ve dodged a bullet. But here you are, three days later, and your neck feels like someone replaced your spine with a rusty hinge.
Sound familiar?
If you live in or around Whitehouse, Texas, you’ve probably driven that stretch of highway more times than you can count. You know exactly where the speed limits change, where people always slam on their brakes, where the merge lanes get dicey. What you might not know is that our seemingly quiet roads see their fair share of fender-benders, rear-enders, and those “how did that even happen” kinds of crashes.
And here’s what nobody talks about at those awkward roadside conversations while you’re exchanging insurance information: car accidents mess with your body in ways that don’t always show up immediately. Your adrenaline is pumping so hard you could probably lift a truck, masking pain that’ll hit you like a freight train once you’re home and trying to sleep.
I’ve been working with folks in East Texas for years, and I can’t tell you how many people shuffle into our clinic weeks – sometimes months – after an accident, looking sheepish and saying something like, “I probably should have come in sooner, but I thought it would just go away.”
That’s the tricky thing about car accident injuries. Your body is basically a really sophisticated shock absorber, and when a couple thousand pounds of metal suddenly stops or changes direction, all that force has to go somewhere. Sometimes it’s obvious – broken bones, cuts, the dramatic stuff you see in movies. But more often? It’s the subtle stuff. The way your shoulder blade won’t stop aching. How your lower back seizes up when you try to get out of bed. The headaches that weren’t there before.
You might be thinking, “But I was only going 25 mph when it happened.” Here’s the reality check: you don’t need to be in some Hollywood-style pile-up to end up dealing with real, persistent pain. Low-speed collisions can absolutely wreak havoc on your musculoskeletal system, especially if you were caught off guard (which, let’s be honest, you always are).
The question isn’t whether you’ll have some discomfort after an accident – it’s whether you’ll address it properly and promptly, or whether you’ll join the ranks of people who still wince when they turn their head two years later, wishing they’d gotten help when it would have made the biggest difference.
Look, I get it. Nobody wants to be that person who makes a big deal out of everything. You don’t want to seem dramatic or weak. Plus, dealing with insurance companies and medical appointments when you’re already stressed? It feels overwhelming. But here’s what I’ve learned from helping hundreds of people navigate this exact situation: taking care of yourself right after an accident isn’t being dramatic – it’s being smart.
In this article, we’re going to walk through everything you need to know about finding the right care after a car accident in Whitehouse. Not the generic, cookie-cutter advice you’ll find on insurance websites, but real, practical guidance about when to seek treatment, what kind of doctor to see, and how to make sure you’re not dealing with preventable pain months down the road.
We’ll talk about those sneaky symptoms that don’t show up until later… the difference between soreness and something that actually needs attention… and yeah, we’ll tackle the insurance maze too, because nobody should have to choose between their health and their bank account.
Because the truth is, the decisions you make in the days and weeks following an accident can literally determine whether you bounce back completely or end up managing chronic pain for years to come.
Your Body’s Hidden Response to Car Accidents
Here’s the thing about car accidents – your body doesn’t always follow the script you’d expect. You might walk away from a fender-bender feeling absolutely fine, maybe even a little proud of how well you handled everything. Then three days later? You can barely turn your neck to check your blind spot.
It’s like your body has this weird delay mechanism built in. Think of it as shock absorber for your nervous system – initially, adrenaline and your fight-or-flight response mask what’s really happening underneath. Your body is essentially saying, “We’ll deal with this later, right now we need to survive.”
The Adrenaline Masquerade
That rush you feel immediately after an accident isn’t just psychological – it’s a powerful cocktail of hormones flooding your system. Adrenaline, cortisol, endorphins… they’re all working overtime to keep you functional in what your brain perceives as a crisis situation.
But here’s where it gets tricky (and honestly, a bit unfair): these same hormones that help you exchange insurance information and call for help are also masking pain signals. It’s like having a really good poker face when you’re actually holding terrible cards.
This masking effect can last anywhere from a few hours to several days. I’ve seen patients who felt completely normal for almost a week before suddenly experiencing severe neck pain, headaches, or back stiffness. Your body was hurt – it just took time for the message to get through.
Understanding Soft Tissue Injuries
When we talk about car accident injuries, we’re usually dealing with what doctors call “soft tissue injuries.” That’s basically everything that isn’t bone – your muscles, tendons, ligaments, and all the connective tissue that holds you together like a well-designed building.
The problem with soft tissue is that it doesn’t show up on X-rays. You could have significant muscle strain, ligament damage, or inflammation that’s completely invisible to traditional imaging. It’s like trying to see a bruise on the inside of an apple – the damage is real, but you can’t spot it from the outside.
The Whiplash Phenomenon
Let’s talk about whiplash for a second, because it’s probably the most misunderstood car accident injury out there. People sometimes roll their eyes at whiplash claims, thinking it’s not “real” or that people are exaggerating. But whiplash is actually a pretty brutal biomechanical event.
Picture your head as a bowling ball (about the same weight, actually) sitting on top of your neck. In a collision, your body stops or changes direction abruptly, but your head keeps moving due to inertia. Then it snaps back in the opposite direction. Your poor neck – which wasn’t designed for this kind of abuse – gets stretched, compressed, and twisted all at once.
The cervical spine has these delicate curves that distribute weight and absorb shock during normal movement. But in a collision, these curves can get straightened out temporarily, putting enormous stress on muscles and ligaments that aren’t built to handle it.
Beyond the Neck: Full-Body Impact
Here’s something that surprises a lot of people – car accidents don’t just affect the obvious areas. Sure, neck and back injuries get most of the attention, but your whole body absorbs the impact forces.
Your shoulders might tense up from gripping the steering wheel. Your lower back could get compressed from the seat belt (which, don’t get me wrong, absolutely saves lives). Even your jaw can get affected if you clench it during impact – something called TMJ dysfunction that can cause headaches and facial pain for months.
Think of it like dropping a pebble in a pond. The initial splash might be at one spot, but those ripples spread outward, affecting areas you wouldn’t expect.
The Time Factor
This is probably the most counterintuitive part of car accident injuries – they often get worse before they get better, even with proper treatment. It’s not that treatment isn’t working; it’s that inflammation and muscle guarding take time to develop and then resolve.
Your body’s initial response is often to tighten up everything around an injured area, like putting internal splints on the damage. This protective mechanism can actually create new problems – muscle spasms, restricted range of motion, and compensation patterns where other parts of your body start working overtime to make up for the injured areas.
That’s why early intervention matters so much, even when you’re feeling okay…
Don’t Wait for the “Big” Symptoms to Show Up
Here’s something most people don’t realize – your body’s basically a master at hiding car accident injuries. It’s like that friend who says they’re “fine” while clearly falling apart inside. The adrenaline from a crash can mask pain for days, sometimes weeks.
I’ve seen patients walk into our clinic three weeks after what seemed like a “minor fender-bender” barely able to turn their heads. They kept waiting for the pain to go away on its own… spoiler alert: it didn’t.
The 72-hour rule is your friend here. If you’re experiencing ANY discomfort – even that weird stiffness that “isn’t that bad” – get checked within three days. Your insurance company will thank you later (seriously, they prefer early intervention over months of treatment down the road).
The Sneaky Symptoms That Actually Matter
You know how everyone talks about whiplash? That’s just the tip of the iceberg. Watch out for these less obvious red flags that often get brushed off
Headaches that feel different – Not your typical stress headache, but something that sits at the base of your skull or behind your eyes. These can signal cervical spine issues that’ll only get worse if ignored.
Sleep problems – If you’re suddenly tossing and turning when you used to sleep like a baby, your nervous system might be processing trauma. This isn’t just “stress” from the accident paperwork.
Brain fog – Can’t concentrate at work? Forgetting where you put your keys more than usual? Even minor concussions can cause these cognitive hiccups that people rarely connect to their car accident.
Tingling or numbness – Anywhere. Your hands, feet, that weird buzzing in your shoulder blade. This suggests nerve involvement, and nerves… well, they’re picky about healing properly.
The Treatment Timeline That Actually Works
Most people approach car accident recovery like they’re waiting for a pizza delivery – they want to know exactly when they’ll feel better. Reality check: healing isn’t that predictable.
Week 1-2: This is crisis management mode. Ice, gentle movement (not bed rest – that’s old school thinking), and getting a professional assessment. Don’t try to “tough it out” yet.
Weeks 3-6: Here’s where the real work begins. Your body’s initial inflammatory response is calming down, but now you need targeted treatment. Physical therapy, chiropractic care, maybe massage therapy if your muscles are still acting like angry teenagers.
Months 2-3: The boring middle phase. You’re probably feeling better some days, worse others. This is normal, but it’s also when people often quit treatment too early. Don’t be that person.
Insurance Navigation (Because Someone Has to Talk About It)
Let’s be real – dealing with insurance after a car accident feels like trying to solve a Rubik’s cube blindfolded. But here’s what they don’t advertise: you have more control than you think.
Document everything. That little voice memo on your phone describing how you feel each morning? Pure gold for your claim. Photos of any visible injuries, even minor bruising. Keep a simple daily pain journal – just a number from 1-10 and a few words about what hurts.
Most insurance policies cover 12-24 physical therapy visits without prior authorization. Use them. Don’t save them for “later” – your body needs help now, not when you’re desperate.
Building Your Treatment Team (It Takes a Village)
Here’s something that might surprise you: one provider usually isn’t enough for comprehensive car accident recovery. Think of it like renovating a house – you wouldn’t expect your plumber to also handle the electrical work.
Start with a primary care doctor or urgent care for initial assessment and documentation. Then consider
– A chiropractor for spinal alignment issues – A physical therapist for movement and strength – A massage therapist for soft tissue work – Sometimes a neurologist if you’re dealing with headaches or cognitive issues
The key is finding providers who actually communicate with each other. Ask if they’ll coordinate your care – the good ones will say yes immediately.
When “Getting Better” Isn’t Linear
Recovery from car accidents is like learning to dance – two steps forward, one step back, occasionally stepping on your own feet. Some days you’ll feel amazing, others like you’ve been hit by a truck all over again.
This doesn’t mean you’re not healing. Your body is literally rewiring itself, rebuilding damaged tissue, and relearning how to move properly. Give it the time and support it needs, and you’ll get there.
The “I Feel Fine” Trap
Here’s the thing about car accidents – your body lies to you. Not maliciously, but it does. That surge of adrenaline? It’s basically nature’s painkiller, and it’s really good at its job. You’ll walk away from a fender-bender thinking you’re invincible, only to wake up the next morning feeling like you wrestled a bear… and lost.
I’ve seen people dismiss serious injuries because they could still move around right after the crash. “But I drove myself home!” they’ll say, as if that somehow proves they’re fine. Your body can mask pain for hours, even days. It’s actually trying to protect you, but sometimes that protection works against your best interests.
The solution isn’t to panic every time you have a minor collision, but don’t let false confidence keep you from getting checked out. If you’re even slightly unsure, see someone within 24-48 hours. Think of it like this – you wouldn’t ignore a strange noise in your car’s engine, right?
When Everyone Becomes a Medical Expert
Oh boy, this one’s frustrating. The minute you mention you were in an accident, suddenly everyone’s got opinions. Your neighbor who watches too much medical TV, your coworker who “had the same thing happen,” your aunt who swears by some miracle cure she saw on Facebook…
“You don’t need a doctor – just ice it and take some ibuprofen!”
“My cousin had whiplash and was fine in three days!”
“Doctors just want to make money off you – walk it off!”
Look, people mean well. They really do. But car accident injuries aren’t one-size-fits-all situations. What worked for Karen from accounting might not work for you. Your spine isn’t the same as your neighbor’s spine, and frankly, most well-meaning advice comes from people who don’t actually understand what happened inside your body during that crash.
Here’s what helps: smile, nod, thank them for caring, then make your own informed decision. You don’t need to justify seeking professional medical care to anyone.
The Insurance Company Maze
Let’s be honest – dealing with insurance after an accident feels like trying to solve a Rubik’s cube while blindfolded. The adjuster wants you to settle quickly (red flag, by the way), you’re not sure what’s covered, and meanwhile, you’re dealing with pain that might be getting worse.
Some insurance companies will actually encourage you to delay treatment, hoping your injuries will resolve on their own. Others might suggest you see their preferred provider – who might not have your best interests at heart.
The smartest move? Get evaluated by someone who works for you, not the insurance company. Document everything. Every symptom, every limitation, every sleepless night. Take photos if you have visible injuries. Keep a simple daily log of how you’re feeling – it doesn’t have to be elaborate, just honest.
And here’s something most people don’t know: in many states, you have protection for medical treatment regardless of who was at fault. Don’t let insurance confusion keep you from getting the care you need.
The “It’s Just Whiplash” Minimization
Whiplash has somehow become the punchline of injury jokes. People roll their eyes when they hear it, like it’s not a “real” injury. This drives me crazy because whiplash – or more accurately, cervical strain – can be absolutely debilitating.
Your neck contains seven vertebrae, countless muscles, ligaments, and nerves. When your head snaps back and forth (which happens in even low-speed collisions), those delicate structures can get seriously disrupted. We’re talking about the bridge between your brain and the rest of your body here.
“Soft tissue damage” might sound minor, but try telling that to someone who can’t turn their head to check their blind spot, or whose headaches are so severe they can’t concentrate at work.
Don’t let anyone – including yourself – minimize what you’re experiencing. If it hurts, it matters. If it’s affecting your daily life, it’s significant. Period.
The Time Crunch Reality
I get it – you’re busy. Taking time off work for medical appointments feels impossible. You’ve got deadlines, meetings, kids to pick up, life to live. But here’s the thing about injuries: they don’t care about your schedule.
Putting off treatment often makes everything take longer in the end. That stiff neck that could have been addressed in a few visits? Let it go for weeks, and you might be looking at months of treatment.
Try to find providers who understand real life – early morning appointments, weekend hours, or clinics that can work with your schedule. Many places are more flexible than you might think, especially when they know you’re dealing with accident-related injuries.
What to Expect After Your First Visit
Here’s the thing about car accident injuries – they’re not like a broken bone where you get an X-ray, see the problem, and know exactly how long healing takes. Your body’s been through trauma, and it’s going to need time to sort itself out.
After your initial evaluation, don’t expect to walk out feeling completely better. I mean, wouldn’t that be nice? But your doctor will likely start with conservative treatments – think ice, gentle movement, maybe some anti-inflammatory medication. The goal isn’t to mask everything immediately; it’s to support your body’s natural healing process.
You might leave with a handful of instructions that seem almost… too simple. “Apply ice for 15 minutes every few hours.” “Gentle neck stretches.” “Avoid heavy lifting.” Trust me, these basics matter more than you’d think. Your body’s like a smartphone after dropping it – sometimes it needs to be turned off and on again, gently.
The Reality of Recovery Timelines
Most people want to know: “When will I feel normal again?” And honestly? It varies so much that giving you a specific timeline would be doing you a disservice.
For minor soft tissue injuries – the kind where you’re sore but functional – you might start feeling significantly better within a week or two. But here’s what nobody tells you: feeling better doesn’t necessarily mean you’re completely healed. Those deeper tissues, the ones you can’t see or feel directly, they’re still doing their work.
More significant injuries… well, they’re playing by different rules. We’re talking weeks to months, not days. And that’s not because something’s wrong with you – that’s just biology. Your muscles, ligaments, and nerves don’t operate on your schedule, unfortunately.
Some days you’ll feel great, then wake up the next morning wondering what happened. That’s normal. Healing isn’t a straight line; it’s more like a stock market chart with ups and downs, but hopefully trending upward over time.
When You’ll Need Follow-Up Care
Your doctor will probably want to see you again in a week or two, depending on your symptoms. This isn’t just a formality – they’re watching for red flags and tracking your progress.
If you’re improving steadily, these visits might become less frequent. But if you’re stuck – not getting worse, but not getting better either – that’s when additional treatments come into play. Physical therapy, maybe some imaging studies, possibly referrals to specialists.
Don’t take it personally if recovery takes longer than expected. Some people bounce back quickly (we all know that person who seems invincible), while others need more time and attention. Neither scenario reflects anything about your character or pain tolerance.
What Happens If You Don’t Improve
Sometimes – and this is the part nobody wants to think about – symptoms persist or even develop weeks after the accident. Late-onset pain isn’t uncommon, especially with injuries like whiplash.
If you’re not seeing improvement after several weeks of appropriate treatment, your doctor might recommend additional testing. MRI scans, nerve conduction studies, maybe consultation with orthopedic specialists or neurologists. This doesn’t mean something’s terribly wrong; it just means you need a more detailed look at what’s happening.
The key is staying in communication with your healthcare team. That nagging headache that won’t quit? The shoulder pain that’s getting worse instead of better? Don’t tough it out – speak up.
Building Your Support Team
Recovery from a car accident often involves more than just your primary doctor. You might work with physical therapists, chiropractors, massage therapists… it takes a village sometimes.
Each professional brings something different to the table. Your physical therapist will help rebuild strength and mobility. A good massage therapist can work out those stubborn knots that seem to have taken up permanent residence in your shoulders.
The important thing? Make sure everyone’s talking to each other. Keep your primary doctor in the loop about other treatments you’re pursuing. Medical care works best when it’s coordinated, not when it’s five different people doing five different things without knowing what the others are up to.
Remember – seeking treatment after a car accident isn’t admitting weakness. It’s giving your body the best possible chance to heal completely, rather than just “getting by” with lingering issues that could affect you for years to come.
You know what? Car accidents are scary enough without having to worry about whether you’re “hurt enough” to see a doctor. And that’s exactly the kind of thinking that keeps so many people suffering in silence – or worse, dealing with complications that could’ve been prevented.
Here’s the thing about your body after a crash… it’s not always going to send you clear signals right away. Sometimes it whispers before it screams. That stiffness in your neck might seem minor today, but your body could be quietly setting up patterns that’ll affect how you move, sleep, and feel for months to come.
I’ve talked to countless people who wished they’d trusted their instincts sooner. The ones who brushed off that “weird feeling” or convinced themselves they were fine because they could still walk around. But here’s what they learned – and what I hope you’ll remember – seeking help early isn’t being dramatic or weak. It’s being smart.
Think about it like this: if your car gets rear-ended, you don’t just glance at it and drive away, right? You check for damage, even the stuff that’s not immediately obvious. Your body deserves at least that same level of attention… probably more, actually, since you can’t trade it in for a newer model.
You Don’t Have to Figure This Out Alone
The beautiful thing about seeing a doctor who specializes in car accident injuries is that they’ve seen it all before. They know how to spot the subtle signs your body might be giving off. They understand the timeline of how these injuries develop – that weird delayed reaction thing isn’t in your head.
And honestly? Even if you go in and everything checks out perfectly fine, isn’t that peace of mind worth it? You’ll sleep better knowing a professional looked at your situation and gave you the all-clear. Plus, you’ll have documentation if something does pop up later (because insurance companies… well, let’s just say they’re not always the most trusting bunch).
The doctors here in Whitehouse who work with car accident patients – they get it. They understand you’re probably feeling overwhelmed, maybe a little anxious about medical bills, possibly questioning whether your symptoms are “real enough” to warrant attention. They’ve helped people navigate all of that before.
Your Next Step (And It’s Easier Than You Think)
Look, I’m not going to tell you that you absolutely must call a doctor right this second – that’s your decision to make. But I will say this: if you’re reading this article, something’s probably nudging at you. Maybe it’s that nagging ache, or the way you’ve been sleeping differently, or just this feeling that something’s not quite right.
Trust that feeling.
You deserve to feel confident in your own body again. You deserve to know what’s going on and what your options are. And you definitely deserve to work with healthcare providers who’ll listen to your concerns without making you feel like you’re overreacting.
If you’re in the Whitehouse area and you’re dealing with any discomfort, changes in how you feel, or just want someone knowledgeable to take a look – reach out. Most car accident specialists offer consultations where they can assess your situation and help you understand what’s happening with your body.
Your health isn’t something to gamble with, and neither is your peace of mind.