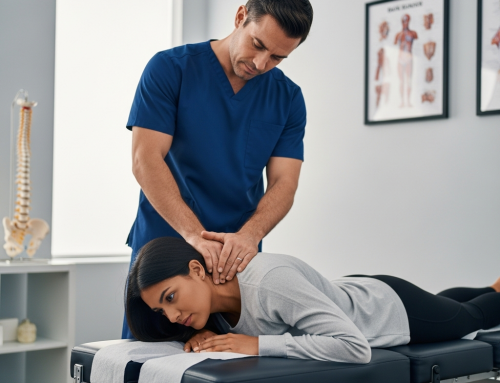
Tyler Car Accident Doctor: What to Expect in the First 30 Days
The coffee mug slips from your hands as the impact jolts through your entire body. One moment you’re singing along to the radio, mentally planning your grocery list… the next, you’re sitting in a crumpled mess of metal and airbag dust, wondering what the hell just happened.
Your hands are shaking – whether from adrenaline or something more serious, you can’t tell. The other driver is walking around, gesturing wildly while talking to someone on their phone. A kind stranger taps on your window, asking if you’re okay. Are you okay?
That’s the million-dollar question, isn’t it?
You wiggle your fingers, rotate your shoulders. Everything seems to work. The paramedics check you out, and besides feeling rattled (and maybe slightly embarrassed), you decline the ambulance ride. “I’m fine,” you tell everyone – including yourself. You exchange insurance information, call a tow truck, and somehow make it home.
But here’s the thing about car accidents… they’re sneaky little devils. What feels like “fine” in those first few hours can morph into something entirely different by tomorrow morning. Or next week. Or – and this happens more often than you’d think – three weeks from now when you wake up and can barely turn your head.
If you’re reading this from Tyler, Texas, chances are you’ve either been in an accident recently or you’re trying to figure out what comes next after one. Maybe you’re that person who said “I’m fine” but now you’re wondering if you actually are. Or perhaps someone you care about is dealing with this, and you want to help them navigate what honestly feels like a confusing maze of medical appointments, insurance calls, and paperwork.
Here’s what nobody tells you about car accidents: the first 30 days are absolutely critical for your recovery, but they’re also the most overwhelming. You’re dealing with insurance adjusters who speak in code, trying to figure out if that persistent headache is “normal,” and wondering whether you should see a doctor when you don’t even know what kind of doctor you need.
I’ve seen this scenario play out hundreds of times. People stumble into our clinic weeks after an accident, frustrated and in pain, saying things like, “I wish I’d known what to expect” or “Nobody told me it could take this long to feel better.” That knot in your stomach? The one that tightens every time you think about medical bills or wonder if you’re overreacting to your symptoms? Yeah, that’s completely normal too.
The truth is, finding the right car accident doctor in Tyler isn’t just about treating injuries – though that’s obviously important. It’s about having someone in your corner who understands the whole messy process. Someone who knows how to document your injuries properly for insurance purposes, who can explain why your neck hurts worse on rainy days now, and who won’t make you feel dramatic for coming in when you’re not even sure anything’s wrong.
Over the next few minutes, we’re going to walk through exactly what you can expect during those crucial first 30 days after your accident. Not the sterile, clinical version you’d find in a medical textbook, but the real deal – the emotions, the paperwork, the 2 AM Google searches about whether headaches after car accidents are serious (spoiler alert: they can be).
We’ll talk about warning signs you shouldn’t ignore, even when they seem minor. We’ll cover what questions to ask potential doctors and what red flags to watch for. You’ll learn about the different types of treatments available and – this is huge – how to work with insurance companies without losing your sanity.
Most importantly, we’ll help you understand that seeking medical care after an accident isn’t admitting weakness or being dramatic. It’s being smart. Because your body just went through something traumatic, and it deserves proper attention and care.
So take a deep breath. You don’t have to figure this out alone, and you don’t have to be perfect at navigating something you’ve hopefully never had to deal with before. Let’s get you the information you need to make the next 30 days as smooth as possible.
Your Body’s Hidden Damage Control Center
Here’s the thing about car accidents – they’re basically like hitting your body with a surprise physics lesson that nobody asked for. One moment you’re cruising down the road thinking about dinner plans, the next you’re dealing with forces that would make Newton proud… and your neck very unhappy.
Your body, bless it, doesn’t exactly send you a detailed injury report right after impact. It’s more like that friend who says “I’m fine!” while clearly bleeding – your adrenaline kicks in, endorphins flood your system, and suddenly you feel like you could run a marathon. Spoiler alert: you probably can’t, and you definitely shouldn’t try.
The Sneaky Nature of Soft Tissue Injuries
Think of your muscles, ligaments, and tendons like a really well-orchestrated rubber band system. When a car accident happens, it’s like someone suddenly yanked all those rubber bands in directions they were never meant to go. Some snap back immediately – ouch, but manageable. Others? They get microscopic tears that whisper “we’ll talk later” before going silent.
Whiplash is probably the most famous of these delayed-reaction injuries, though honestly, the name makes it sound way more dramatic than the actual mechanism. Your head basically becomes a bobblehead for a split second – your body stops with the car, but your noggin keeps moving forward, then snaps back. It’s not pretty, and the resulting neck strain often takes 24-48 hours to really announce itself.
But here’s what’s counterintuitive (and frankly, kind of annoying): the severity of the accident doesn’t always correlate with injury severity. I’ve seen people walk away from dramatic-looking crashes feeling fine, while someone who got rear-ended at 15 mph in a parking lot ends up with weeks of neck pain. Physics is weird like that.
When Your Body Goes Into Shock Mode
After an accident, your body essentially hits the panic button and floods your system with stress hormones. It’s like your internal alarm system got stuck in the “fire drill” position. This can mask pain for hours or even days – which is both a blessing and a curse.
The blessing part? You’re not writhing in agony immediately after impact. The curse? You might make decisions (like refusing medical attention) based on how you feel in those first few hours, which… well, that’s a bit like judging a book by reading only the first sentence.
Your nervous system also gets a bit scrambled. Think of it like your body’s communication network suddenly has really bad cell service – messages about pain and injury might take a while to get through clearly.
The 72-Hour Rule (And Why It Matters)
Most car accident doctors will tell you about the magical 72-hour window, and there’s actually solid science behind it. This is roughly how long it takes for inflammation to really ramp up and for your body’s initial shock response to wear off.
During these first three days, you might experience what I call the “injury crescendo” – symptoms that start quietly and gradually get louder until they’re impossible to ignore. Your stiff neck on day one might become a full-blown headache and shoulder pain symphony by day three.
Actually, that reminds me of something important – headaches after car accidents aren’t always about hitting your head. Sometimes they’re tension headaches from your neck muscles going haywire, or even from jaw clenching (apparently, getting rear-ended makes people unconsciously clench their jaws… who knew?).
Why “Wait and See” Isn’t Always Wise
There’s this temptation to tough it out – especially if you’re dealing with insurance companies or worried about medical bills. I get it, I really do. But here’s the tricky part about soft tissue injuries: they’re like that leak in your roof that seems minor until you realize it’s been slowly damaging everything underneath.
Early intervention doesn’t just help with pain – it can prevent compensation patterns where your body starts moving differently to avoid discomfort, which then creates new problems down the line. It’s like favoring a sore ankle and then developing hip pain because you’ve been walking funny for weeks.
The goal isn’t to turn you into a medical anxious mess, but rather to help you understand that taking car accident symptoms seriously – even mild ones – isn’t being dramatic. It’s being smart.
The Real Story About Day-One Documentation
Here’s something most people don’t realize until it’s too late – that first doctor’s visit after your accident? It’s basically creating your medical roadmap for the next month. Your doctor isn’t just checking if you’re okay; they’re building a case file that insurance companies will scrutinize with a magnifying glass.
Bring a list. I know, I know – you’re probably thinking “I’ll remember everything,” but trust me on this. Pain has a funny way of making your brain foggy. Write down every single thing that feels different – that weird shoulder twinge when you reach for coffee, the headache that wasn’t there yesterday, even if your sleep feels “off.” Insurance adjusters love to claim that symptoms appearing later aren’t related to the accident. Don’t give them that ammunition.
Week Two Reality Check (When the Adrenaline Wears Off)
This is where things get interesting… and by interesting, I mean potentially frustrating. Around day 10-14, your body starts sending you the real bill for what happened. That stiffness you brushed off? It might bloom into something that makes getting out of bed feel like a negotiation.
Don’t skip your follow-up appointments. Even if you’re feeling better. Actually, *especially* if you’re feeling better. I’ve seen too many people cancel appointments because they had a good day, only to have symptoms resurface weeks later with no medical documentation to back them up.
And here’s a pro tip your doctor might not mention – keep a daily symptom journal. Nothing fancy. Just a quick note in your phone: “Neck stiff in morning, better after shower. Headache around 3 PM.” These patterns matter more than you think.
The Physical Therapy Dance (And Why Timing Matters)
If your doctor recommends PT, don’t wait. There’s this magical window – usually within the first two weeks – where your body is most responsive to treatment. Wait too long, and those muscles start setting into protective patterns that are harder to undo later.
But here’s what they don’t tell you about PT in those early days: it might make you feel worse before you feel better. Your therapist is essentially asking injured tissues to start working again. It’s like asking someone with a sprained ankle to start walking – necessary, but not always comfortable.
Choose your PT clinic wisely. Ask your doctor for specific recommendations, not just “find a physical therapist.” Some clinics specialize in auto accident injuries and understand the unique challenges you’re facing. Others… well, let’s just say there’s a difference between treating a weekend warrior’s tennis elbow and helping someone recover from whiplash.
Managing the Insurance Maze (While You’re Still Healing)
This part feels overwhelming, but here’s the thing – insurance companies are counting on you being too overwhelmed to stay organized. Don’t let them win.
Get copies of everything. Every report, every test result, every doctor’s note. Create a simple folder (digital or physical) and put everything there. When the insurance adjuster calls asking about that MRI from two weeks ago, you’ll have it at your fingertips instead of scrambling through paperwork while trying to remember which doctor ordered what.
And about those insurance company doctors… if they want you to see their “independent” examiner, remember that this doctor works for them, not you. Be honest, but don’t downplay your symptoms trying to be tough. These appointments typically last 15-20 minutes – barely enough time to understand how your injuries affect your daily life.
Red Flags You Shouldn’t Ignore
Some symptoms deserve immediate attention, even if they seem unrelated to your accident. Persistent headaches that get worse instead of better, vision changes, dizziness that doesn’t improve, or any numbness or tingling in your arms or legs. Your brain got jostled around too, and sometimes the effects don’t show up immediately.
Sleep problems are huge – and often overlooked. If you’re suddenly having trouble falling asleep or staying asleep, mention it to your doctor. Pain disrupts sleep, but so does the stress and anxiety that often follow accidents. Poor sleep slows healing, creates a vicious cycle.
Building Your Recovery Team
Think of your first 30 days as assembling your support crew. You’ve got your primary doctor, maybe a specialist or two, possibly a physical therapist. But don’t forget about the less obvious team members – a good chiropractor who works with auto accident cases, maybe a massage therapist, even a counselor if you’re dealing with anxiety about driving.
The goal isn’t to see every practitioner in town. It’s about building a coordinated team that actually talks to each other about your care.
When Your Body Doesn’t Follow the Timeline
Here’s what nobody tells you: healing isn’t linear. You might feel pretty good on day five, then wake up on day eight feeling like you got hit by… well, another car. It’s maddening, really – especially when well-meaning friends keep asking “Aren’t you better yet?”
Your body’s working overtime to repair itself, and some days it’s going to demand more rest, more care, more patience than you planned to give. That stiffness that seemed manageable yesterday? Today it might make getting out of bed feel like climbing Mount Everest.
The solution isn’t to push through (though I know you’re tempted). Instead, think of recovery like tending a garden – some days you water, some days you prune, some days you just… wait. Keep a simple pain journal on your phone. Rate your discomfort 1-10 each morning and evening. This gives your Tyler car accident doctor real data to work with, not just “I think I’m worse.”
The Insurance Maze Nobody Warned You About
Let’s be honest – dealing with insurance after a car accident feels like trying to solve a Rubik’s cube while wearing mittens. They’ll ask for documentation you didn’t know existed, request records from appointments you forgot about, and somehow make you feel guilty for getting medical care after being injured.
You’re going to get calls. Lots of them. Some days it’ll feel like a part-time job just managing the paperwork and phone calls. And here’s the kicker – while you’re trying to heal, you’re also expected to become an expert in medical billing, policy coverage, and legal terminology.
Start a dedicated email folder for all accident-related correspondence right now. Screenshot everything on your phone – insurance cards, policy numbers, claim numbers, contact information. Create a simple spreadsheet (or even just a note on your phone) tracking who you talked to, when, and what was discussed.
Most importantly? Don’t handle insurance calls when you’re having a bad pain day. Your cognitive function might be compromised, and you don’t want to agree to something you’ll regret later.
The Emotional Rollercoaster You Didn’t See Coming
This one catches everyone off guard. You expected the physical pain, maybe even anticipated some inconvenience… but the emotional aftermath? That hits different.
Some days you’ll feel angry – at the other driver, at your situation, at how long everything takes. Other days, you might feel anxious about driving again or even being a passenger. There’s this weird guilt that creeps in too, especially if others were involved or if you feel like you’re “taking too long” to recover.
And then there’s the isolation. When you can’t do the activities you used to enjoy, when friends stop checking in as regularly, when your world suddenly shrinks to medical appointments and rest days… it’s lonely.
Here’s what helps: acknowledge that this emotional response is completely normal. Your nervous system just went through trauma – of course you’re going to feel unsettled. Consider talking to a counselor who specializes in accident recovery. Many Tyler car accident doctors can provide referrals, and it’s often covered by your auto insurance.
When Work Becomes Complicated
Nobody prepares you for how exhausting it is to explain your limitations over and over. Your boss might be understanding at first, but by week three, you can sense the subtle shift in their patience. Coworkers start making comments about your “extended vacation.”
The truth is, you might look fine from the outside while feeling terrible on the inside. Soft tissue injuries don’t come with visible casts or crutches – they’re invisible disabilities that others struggle to understand.
Document everything with HR. Even if your workplace is supportive, having written records of your restrictions, modified duties, and medical appointments protects everyone involved. Don’t be a martyr – if your doctor says you need restrictions, follow them. Pushing too hard too early often extends recovery time.
The Financial Reality Check
Medical bills start arriving while you’re still figuring out how to sleep comfortably. Time off work means reduced income right when expenses are increasing. It’s a cruel irony that getting injured costs money you might not have.
Create a simple tracking system for all accident-related expenses – medical bills, transportation to appointments, even parking fees. These details matter for insurance claims and potential legal proceedings. Many Tyler car accident doctors understand these financial pressures and may offer payment plans or work directly with your insurance to minimize upfront costs.
Remember: asking about costs upfront isn’t embarrassing – it’s smart planning.
What’s Actually Normal in Those First Few Weeks
Here’s the thing about car accident recovery – it’s messy, unpredictable, and rarely follows the neat timeline you’d expect. Your body doesn’t check a calendar before deciding when to feel better.
In the first week or two, you might feel worse before you feel better. That’s completely normal, actually. Your adrenaline’s wearing off, inflammation is setting in, and your body’s finally getting the memo about what happened. Don’t panic if you wake up on day three feeling like you got hit by… well, a car. Again.
Some people bounce back in a few days. Others need weeks or even months. There’s no “right” way to heal, and comparing yourself to your neighbor who walked away from their fender-bender like nothing happened? That’s just going to make you feel worse.
The Paperwork Dance (Because There’s Always Paperwork)
Your Tyler car accident doctor will be documenting everything – and I mean everything. Every appointment, every symptom, every treatment. This isn’t just for your medical records… it’s building a paper trail that might be crucial if insurance gets complicated down the road.
You’ll probably need to:
– Keep a symptom diary (even when you don’t feel like it) – Track your pain levels daily – Document how injuries affect your daily activities – Save all receipts related to your treatment
I know it’s tedious when you’re already dealing with pain and stress, but think of it as insurance for your insurance claims.
Managing the Insurance Marathon
Speaking of insurance – buckle up. This part can be more exhausting than the actual recovery sometimes. Your doctor’s office will help coordinate with insurance companies, but you’ll still need to stay on top of things.
Personal injury protection (PIP) in Texas typically covers the first $2,500 of medical expenses, regardless of who caused the accident. After that? It gets more complicated. Your doctor’s billing team will work with both your health insurance and the at-fault driver’s insurance, but there might be delays, denials, and general bureaucratic nonsense to navigate.
When to Worry (And When Not To)
Most car accident injuries follow predictable patterns. Whiplash symptoms often peak around 48-72 hours after the accident. Bruising might show up days later. Sleep problems? Super common in the first few weeks.
But you should definitely call your doctor if you experience
– Sudden, severe headaches that won’t respond to medication – Numbness or tingling that’s getting worse – Vision problems or dizziness that persists – Memory issues beyond normal post-accident fog
On the flip side, don’t freak out if you’re still sore after two weeks. Or if you’re more emotional than usual – trauma affects everyone differently, and your brain is processing a lot right now.
Building Your Support Team
Recovery isn’t a solo sport. Beyond your Tyler car accident doctor, you might need a whole crew: physical therapists, massage therapists, maybe even a counselor if the emotional impact is significant.
And don’t forget about the people in your life. Let your family and friends help. Accept the casserole. Say yes when someone offers to drive you to appointments. This isn’t the time to be a hero about independence.
Looking Ahead (Realistically)
Most minor to moderate car accident injuries resolve within 6-12 weeks with proper treatment. But “resolve” doesn’t always mean “completely back to normal.” You might have some lingering stiffness on rainy days, or need to be more mindful about your posture going forward.
That’s not failure – that’s just life after trauma. Your body has been through something significant, and sometimes it holds onto that experience in small ways.
The goal isn’t to pretend the accident never happened. It’s to get you back to living your life fully, even if that life looks slightly different than before. Some of my patients say they’re actually more in tune with their bodies after going through this process… there’s something to be said for that level of awareness.
Your Tyler car accident doctor will work with you to set realistic goals and adjust the treatment plan as you heal. Recovery isn’t linear, and the best doctors know that. Trust the process, listen to your body, and give yourself permission to heal at your own pace.
You Don’t Have to Figure This Out Alone
Here’s something nobody tells you about those first 30 days after a car accident – they’re going to feel like a strange mix of slow motion and fast-forward all at once. One minute you’re lying awake at 3 AM wondering if that ache in your shoulder is normal, the next you’re suddenly three weeks out and realizing you’ve been compensating for pain without even thinking about it.
Your body has this incredible ability to adapt… sometimes too well. That slight limp to avoid putting weight on your sore hip? It becomes second nature before you know it. And while your body’s trying to protect itself, other areas start working overtime to pick up the slack. It’s like when one person calls in sick at work – everyone else scrambles to cover, but they can’t keep that pace forever.
The thing is, what feels manageable in week one can snowball into something much bigger by week four if you’re not paying attention. I’ve seen it happen countless times – people who thought they were “tough enough” to push through, only to find themselves dealing with chronic issues months later that could have been addressed early on.
But here’s what I want you to remember: getting help isn’t admitting defeat. It’s not being dramatic or weak or any of those things that stubborn voice in your head might be whispering. Actually, it’s quite the opposite – it’s being smart about your long-term health and quality of life.
Think about it this way… you wouldn’t ignore a warning light on your car’s dashboard for weeks, right? Your body has warning lights too, and they’re worth paying attention to. That persistent headache, the stiffness that’s not getting better, the way you’re sleeping differently – these aren’t necessarily “normal” parts of recovery.
The medical professionals who specialize in car accident injuries? They’ve seen it all. They understand the timeline of healing, they know which symptoms are red flags, and they can spot potential problems before they become bigger issues. More importantly, they won’t make you feel silly for coming in, even if you’re not sure whether something is “serious enough.”
Ready to Take the Next Step?
If you’re reading this and something’s nagging at you – whether it’s physical discomfort, concerns about your recovery, or just wanting someone knowledgeable to tell you that what you’re experiencing is normal – don’t wait. Those first 30 days are precious time when your body is most responsive to treatment and intervention.
We’re here whenever you’re ready. No pressure, no judgment, just genuine care for helping you feel like yourself again. You can call us, send a message, or even just stop by to chat about what you’re experiencing. Sometimes just talking through your concerns with someone who understands can provide the clarity and peace of mind you need.
Your recovery matters, and so do you. Let us help make sure you’re setting yourself up for the best possible outcome – not just for the next few weeks, but for the months and years ahead.